
Referrals are a core part of how healthcare works in Australia.
They connect general practice to specialist care, quietly, routinely, and often without much attention.
But if you stop and think about it for a moment, there’s a simple question that doesn’t always have a clear answer:
What actually happens after a referral is sent?
On paper, it’s straightforward. A GP identifies the need, sends the referral, and the patient moves forward.
In reality, it’s a bit messier than that.
A referral might be received and actioned straight away. Or it might sit in an inbox for a while. Sometimes it needs a follow-up. Occasionally, it never quite turns into an appointment at all.
And most of the time, no one really knows, or at least not until a patient calls back to check what’s going on.
If you’ve ever had to ring a specialist clinic just to confirm whether something was received, you’ll know how common such situations are.
In most cases, it’s not that the system fails. It’s that no one has full clarity or visibility of it end-to-end.
What this looks like in Practice
Before getting into what can be done to improve things, let's step back for a second to see what statistics say:
- Around 40% of Australians see a specialist each year, usually through GP-led pathways
- Close to 1 in 5 people delay or miss specialist care when they need it
-
Wait times can range from a few weeks to several months, depending on the service
The pattern becomes clearer when we look at this chart:
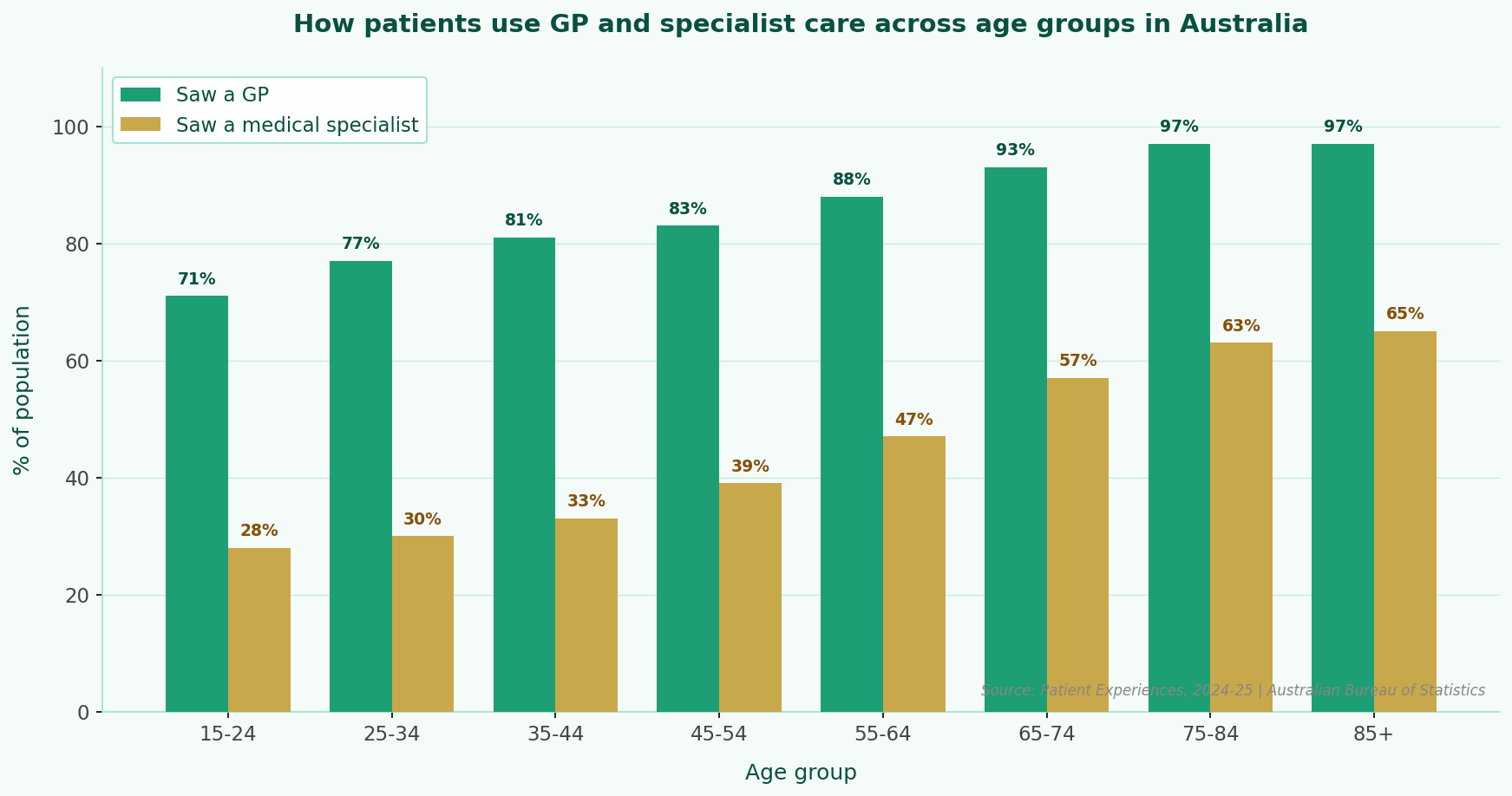
Ref: Patient
Experiences, 2024-25 financial year | Australian Bureau of Statistics
As patients age, reliance on specialist care increases, thereby highlighting the importance of clear, well-functioning referral pathways between GPs and specialists.
But while this pathway becomes more critical over time, what happens between each step isn’t always visible.
So if you’re trying to increase referrals, what actually helps?
It’s easy to assume the answer is more outreach. More networking. More visibility with local clinics.
And yes, that plays a role.
But in practice, referrals tend to follow something much simpler.
If a GP knows a process works consistently, they're far more likely to come back to it.
So it’s worth looking at what actually makes these pathways work.
Where referral pathways usually break and how to fix them
In most cases, it’s not one big issue. It’s a series of small gaps that add up over time.
1. Make it easy to refer — genuinely easy
Most GPs aren’t comparing multiple specialists in detail.
They’re making decisions in the middle of a busy clinic, often between patients.
Even small inconsistencies like different forms, unclear instructions, or extra steps can make the process harder than it needs to be.
And friction, even small amounts, changes behaviour.
Clarity and consistency matter more than optimisation.
That’s usually enough to make you the default choice — especially when GPs know they can rely on the experience each time.
2. Let clinics know it’s been received
Silence is one of the biggest issues here.
Something is sent… and then nothing.
From the GP’s side, that creates uncertainty. Was it received? Is it being actioned?
Even a simple acknowledgement helps.
A small signal can prevent a lot of follow-up.
It also reassures clinics that there’s an active process on the other end — not just a one-way handoff.
3. Close the loop after the patient is seen
Once the patient has been seen, communication tends to drop off. This part is often overlooked.
But for GPs, this stage is where clarity matters most. A short summary. A clear next step.
Referrals aren’t just transactional. They’re relational.
When GPs consistently hear back and feel included in the patient’s journey, trust builds over time, and that’s what drives repeat referrals.
4. Look at how things are handled once they arrive
Not all delays come from outside the system.
Sometimes the bottleneck is internal: requests sitting in inboxes, delays in triaging, or unclear responsibility for follow-up. None of these are major issues on their own. But together, they add friction that patients and referring clinics both feel, even if they can't quite name it.
A more consistent internal flow removes uncertainty.
And when things are easier to manage internally, the experience becomes more predictable for the clinics referring to it.
5. Make the process visible (& not just communicative)
Effective communication tells people what happened. Visibility shows them what's happening now.
Has the referral been received? Is it waiting to be reviewed? Has the patient been booked?
Without that, everything becomes just reactive. GPs follow up, patients call to check, and clinics spend time chasing rather than caring.
Visibility reduces chasing, duplication, and delays.
And when GPs don’t have to follow up or guess what’s happening, they’re much more likely to trust and 'reuse' the same pathway.
6. Don’t lose sight of the patient experience
The patient is at the centre of all these discussions.
Patients don't see whether a referral was received or triaged. They just feel the delay. That uncertainty shapes how patients view the specialist and the GP who referred them.
When the experience is smooth, trust builds across the entire pathway.
And often, that’s what keeps referrals consistent over time. Patients feel more confident. They're more likely to follow through, return, and recommend.
To sum up...
Referrals are a routine part of care, but what happens after they’re sent is what shapes the outcome.
When pathways are clearer, the process becomes easier to trust. And when engagement with GPs is consistent, that trust builds over time. Together, those two things make a noticeable difference.
Not just in how smoothly patients move through care, but in how reliably referrals continue to flow.
Improving referrals often comes down to making the process clearer and staying connected with the GPs you work with.
At RxTro, we focus on helping providers establish more consistent referral pathways.









 AUS
AUS can
can